Keratoconus
What Is Keratoconus?
Keratoconus is a progressive genetic eye disorder that causes thinning of the cornea. It is the most common corneal dystrophy. According to the National Eye Institute, keratoconus affects one in every 2,000 (1/2,000) Americans. This is a disease that affects teenagers and people in their 20s.
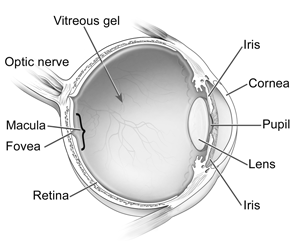
Keratoconus is a non-inflammatory thinning and steepening of the middle of the cornea. This progressive thinning causes a bulge to develop in the normally round cornea. Because the cornea focuses light on the retina, the changing shape of the cornea has a significant impact on your ability to see clearly.
Photo Credit: National Eye Institute, National Institutes of Health
The first symptom of keratoconus is usually a blurring in your distance vision. This mild nearsightedness is usually accompanied by mild astigmatism, the inability of your eye to focus at various focal lengths. It may also be accompanied by increased sensitivity to light and glare.
At this stage, the vision problems can be corrected with eyeglasses or contact lenses. However, because this is a progressive disease, the cornea will continue to thin and you may notice that your current prescription is no longer sufficient. You may also experience headaches from eye strain, particularly after reading.
Keratoconus can affect one or both of your eyes. As the disease progresses over 5-10 years, you will usually experience frequent changes in your astigmatism correction. At that point, your eye will normally stabilize. However, in some patients, the progression of the corneal thinning can be rapid.
Who Is at Risk for Keratoconus?
Although the causes of keratoconus are not fully understood, it is a disease that affects teenagers and people in their 20s. Studies have shown that approximately 7 percent of people with the disease have a family history of keratoconus. Other theories include overexposure to sunlight, improperly fitted contact lenses and chronic eye irritation or eye rubbing. Certain eye diseases including retinitis pigmentosa, and systemic diseases including Down syndrome, are also linked to keratoconus.
If you are a teenager or young adult, or if you are a parent of a teenager, you should take notice of blurry vision and frequently changing prescriptions for glasses and contact lenses. If you notice any instability in your or your child’s vision, a comprehensive eye exam is required. Early detection and treatment may help prevent vision loss.
How Is Keratoconus Detected?
Your doctor will use a slit lamp examination to detect keratoconus. In addition, he may also measure the thickness of your corneas using a pachymeter. A topographical map of your cornea may also be needed to diagnose keratoconus. The corneal topography computer detects irregularities on the corneal surface and shows the amount of irregular astigmatism in keratoconus. Newer technologies include the Orbscan and Pentacam.
How Is Keratoconus Treated?
Eyeglasses or soft contact lenses are the treatment for early keratoconus. As the disease progresses, you may wish to consider rigid gas permeable contact lenses, a type of hard contact lens that may fit better over the irregular shape of your cornea. However, these lenses may be more uncomfortable to wear than soft lenses, and they are more difficult to fit. You will need to be patient and work with your contact lens provider to find the right lens for you.
In 2004, the FDA approved the use of Intacs corneal implants to treat keratoconus. These implants are surgically placed under the surface of your eye, at the side of the cornea. Because they are rigid, they help to flatten the cornea and improve vision, although you will still need to wear glasses or contact lenses. They can also be removed or changed, as your cornea continues to thin. However, they are not a cure for keratoconus.
Another promising new treatment for keratoconus is called C3-R, corneal collagen cross-linking riboflavin. Eyedrops containing riboflavin are placed on your eye and activated by a special light. This helps to strengthen the collagen under your eye and may help your cornea maintain its shape. Early studies show this to be very promising and it may be used in conjunction with corneal implants for maximum effect.
However, if your keratoconus continues to progress and you are no longer able to function with glasses or contact lenses, a corneal transplant may become necessary. Even after a corneal transplant, called a penetrating keratoplasty, you may still need to wear glasses or contact lenses for maximum vision improvement.