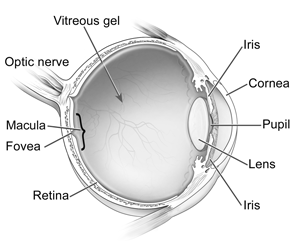
Macular Pucker
What Is a Macular Pucker?
A macular pucker is scar tissue that has formed on the macula, the center of the retina which is responsible for your fine, detailed vision. The cells of the macula, known as photoreceptors, convert light to electrical images. The retina then sends these images via the optic nerve to the brain. A healthy macula allows you to do the daily activities you take for granted such as driving, reading, sewing and other detailed work.
Photo Credit: National Eye Institute, National Institutes of Health
The vitreous gel is the fluid that fills your eye and is attached to the surface of the retina. As you get older, the vitreous changes shape and begins to shrink, pulling away from the retina. Natural fluids will fill this area, and you may notice an increase in floaters, small flecks that appear in your field of vision. This is normal and for most people, this will not cause a problem.
Sometimes, when the vitreous pulls away from the retina, it can cause microscopic damage to the retina’s surface. As the retina attempts to heal the damage, scar tissue called an epiretinal membrane forms. This membrane is firmly attached to the retina. Epiretinal membranes can also form from pieces of the vitreous gel that remain on the retinal surface. The scar tissue can then contract, causing the retina to wrinkle or “pucker”. When this puckering occurs in the macula, the area of the retina responsible for clear central vision, it can cause blurry vision or straight lines may appear wavy.
Most macular puckers are related to vitreous detachment, which usually occurs in people over age 50. As you age, you are at increased risk for macular pucker.
A macular pucker can also be triggered by certain eye diseases and disorders, such as a detached retina and inflammation of your eye (uveitis). Also, if you are a diabetic, you may develop an eye disease called diabetic retinopathy, which can cause a macular pucker. A macular pucker can also be caused by trauma from either surgery or an eye injury.
A macular pucker and age-related macular degeneration are two separate and distinct conditions, although the symptoms for each are similar. In addition, a macular pucker and a macular hole are different conditions, although they both are caused by shrinking in the vitreous that pulls on the retina, and have similar symptoms - distorted and blurred vision. If the pulling is slight and only causes microscopic damage, your retina may heal itself, although scar tissue or a macular pucker may form. However, if the shrinking vitreous pulls too hard, a macular hole can form. This is a more serious condition.
The severity of vision loss can vary, although severe loss of vision from a macular pucker is not common. You may experience difficulty in doing close up, detailed work such as reading or sewing. In some cases, a small blind spot in your central vision may also develop.
Who Is at Risk for a Macular Pucker?
As people age, everyone is at risk of developing a macular pucker. It is more likely to occur in people over the age of 50.
How Is a Macular Pucker Detected?
A macular pucker is diagnosed during a comprehensive eye examination, which will include:
- Visual acuity test: Testing your vision at various distances
- Dilated eye exam: Examining your retina and the back of your eye
- Tonometry: Measuring your intraocular pressure
Your doctor may also suggest special tests, called fluorescein angiography or optical coherence tomography (OCT). These tests provide detailed pictures of your retina.
How Is a Macular Pucker Treated?
In most cases, no treatment is required for a macular pucker. Like most people, you may be able to adapt to the vision loss or distortion in mild cases. There are no medications or nutritional supplements that will improve any vision loss you experience from a macular pucker. In some, rare cases, the scar tissue may separate from the retina and your vision will clear up.
If your vision loss is severe, a surgical procedure called a vitrectomy may be recommended to remove the vitreous gel and scar tissue that are pulling on your retina. This procedure is performed by our highly experienced retina specialist. (For more information on retinal operations in our surgery center, please click here.)
Our retina specialist uses 25-gauge transconjunctival sutureless vitrectomy techniques. This method uses the most advanced technology to perform this type of surgery, leading to a more comfortable post-operative course with faster recovery times. (For more information on this procedure, please click here.)
The procedure will be done under local anesthesia, and you will also be given a mild sedative. Your eye will be completely numbed and you will remain comfortable during your surgical experience.
You should not eat or drink anything after midnight the night before your procedure. On the day of treatment, you will be welcomed by a staff member. The staff will help you prepare for your surgery by putting eye drops in your eye. You will be given a gown to wear over your street clothes during your actual surgery.
After your surgery, you will rest in a comfortable reclining chair. Your family members may then join you in reviewing your follow-up care and schedule. You may be given medication or eyedrops to prevent infection and inflammation. Your surgeon will see you the next day after surgery to check how your eye is healing.
After the operation, you will need to wear an eye patch for a few days to protect and help the eye heal. You will also need to use medicated eye drops to protect against infection and inflammation.
Any surgical procedure involves some risks. These risks include infection, bleeding, retinal detachment and accelerated cataract formation. Also, the macular pucker may grow back, but this is rare. However, most of these conditions can be successfully treated. The potential risks associated with a vitrectomy are less than the expected benefits of preserving your vision.
Surgery to repair a macular pucker is very delicate, and while vision improves in 90 percent of cases, your vision may not return to normal. On average, about half of the vision lost from a macular pucker is restored. In most cases, the distortion in your vision is significantly reduced, although this recovery can take up to six months or more. You should talk with your retinal specialist about whether treatment is appropriate.
Because macular puckers are a function of aging, as are a number of other age-related disorders including glaucoma and macular degeneration, we recommend annual eye examinations beginning at age 55. Please do your part to protect your vision!
Macular Pucker Specialist at Kadrmas Eye Care New England
Meet our ophthalmologist who specializes in the treatment of macular degeneration: