Retinal Vascular Venous Disease
What Is Retinal Vascular Venous Disease?
Retinal venous occlusion is an obstruction in the system of veins that drain blood away from the retina. There are two types of retinal vein occlusions: Branch retinal vein occlusion (BRVO) and central retinal vein occlusion (CRVO). In the United States, retinal vein occlusions are the second most common retinal vascular disease after diabetic retinopathy.
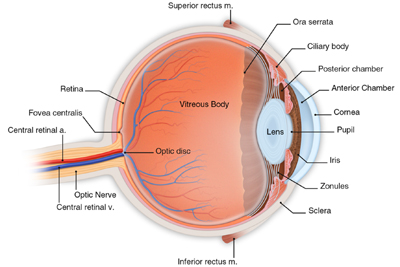
The central retina artery and branch arteries pump blood and nutrients to the retina, while the central retinal vein and branch veins carry blood and waste products out of the eye. Capillaries are very thin, fragile vessels embedded in tissue that connect the arteries and veins. Although they are fragile, capillaries play a critical role in allowing the nutrients from the arteries to nourish the retina and to allow the waste products to flow into the veins. This retinal vascular system requires all parts to be functioning properly for you to see clearly.
What Is Branch Retinal Vein Occlusion (BRVO)?
If your vascular system is functioning properly, the blood from the smaller branch veins will flow through one of the larger branch veins into the central retinal vein seen above. However, sometimes when an artery becomes hardened and is pressing down on an adjacent branch vein, the blood will not drain properly. When blood starts to collect in a branch vein, it increases pressure on the capillaries. This increased pressure will cause the capillaries to hemorrhage and leak blood onto the retina. This leakage can permanently damage the capillaries and impact the retina’s ability to absorb nutrients.
In addition, if a significant area of capillaries is involved, the occlusion is considered ischemic. Ischemia impacts the retina’s ability to circulate blood and to obtain an adequate supply of oxygen. This process will also release chemicals that will stimulate neovascularization, the proliferation of weak, immature blood vessels on the surface of the retina. These immature blood vessels can also continue to leak or bleed.
Although in some cases branch retinal vein occlusion can improve without treatment, BRVO can lead to vision loss and macular edema. If BRVO is ischemic, acute vision loss is possible. If neovascularization develops, the abnormal blood vessels can bleed into the vitreous cavity, causing floaters and loss of vision.
If you have BRVO, you may notice a rapid, painless decrease in vision in one eye. This may also be accompanied by a scotoma or blind spot, an isolated area of diminished vision. You may also have a decrease in your peripheral or side vision.
Who Is at Risk for Branch Retinal Vein Occlusion (BRVO)?
The Eye Disease Case-Study noted that people with hypertension (high blood pressure) are at high risk for developing branch retinal vein occlusion. Recent studies in the United Kingdom also note that there is an association between being diabetic and developing retinal vein occlusion. This may be linked to the fact that approximately 70 percent of diabetics have hypertension. A recent Japanese study has also shown a linkage between glaucoma and BRVO. BRVO is more common in people over age 50.
What Is Central Retinal Vein Occlusion (CRVO)?
Central retinal vein occlusion is caused by an obstruction to the central retinal vein. The central retinal vein is the main vein that removes waste products from the eye.
CRVO is divided into two types: Non-ischemic and ischemic. Non-ischemic is the less serious type of central retinal vein occlusion and is the more common type in the United States. Initially, there may be little impact on your vision. Ischemic CRVO is more serious and can either occur on its own or evolve from non-ischemic. Ischemic CRVO will usually be accompanied by a serious change in your vision.
The cause of CRVO is the subject of debate. However, the central retinal vein and arteries share a common vessel or sheath as they exit the optic nerve. Any compression or damage to this sheath can cause an occlusion in the vein. Also, a thrombus or clot may form in the central retinal vein causing the blockage. Such a blockage results in a backup of blood in the retina, which can lead to the production of the hormone that stimulates neovascularization. This hormone is called vascular endothelial growth factor or VEGF, for short. In addition to stimulating neovascularization, VEGF can also increase leakage in the capillaries which can lead to macular edema.
In its initial stages, there may be little or no impact on your vision. However, it is also possible for vision loss to be rapid. As the disease progresses, your vision will continue to deteriorate without treatment and you may notice an increasing level of discomfort and redness, if intraocular pressure rises due to neovascularization.
If you have a central retinal vein occlusion, the neovascularization can lead to a vitreous hemorrhage and potential retinal detachment. If the neovascularization occurs on the iris, it can lead to neovascular glaucoma, the most serious complication of CRVO. Thus CRVO can have serious implications for your vision.
Who Is at Risk for Central Retinal Vein Occlusion (CRVO)?
Just as with BRVO, a history of hypertension, diabetes and glaucoma are risk factors for central retinal vein occlusion. Other risk factors also include cardiovascular or clotting disorders.
Both men and women are at risk for CRVO, although it is slightly more common in men. Although CRVO can affect any age group, 90 percent of the time it occurs in people over age 50. If you have had CRVO in one eye, there is about a 20 percent chance that it will occur in the other eye.
How Are BRVO and CRVO Detected?
BRVO and CRVO are detected through a comprehensive eye examination, including:
- Ophthalmoscope examination
- Visual acuity test
- Slit lamp exam
- Gonioscopy
- Fluorescein angiogram
- Optical coherence tomography
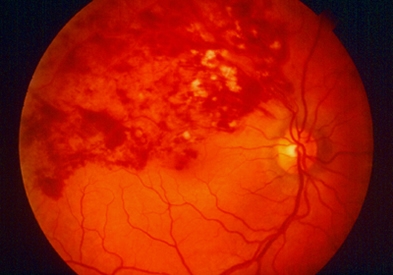
Your doctor will be able to examine the extent of vein occlusion and its location in your eye. For example, in the picture of BRVO, you can see the extent of hemorrhaging localized in the branch veins. The central retinal vein is unaffected.
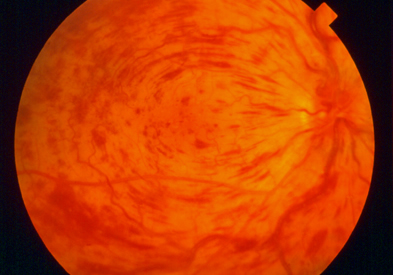
However, in the CRVO example, hemorrhages are present in all four quadrants of the retina, corresponding to the major branches out of the central retinal vein. Much more of the retina is involved and this is more likely to have more significant impact on your central and peripheral vision.
Once your doctor has carefully examined your eye and your test results, he will discuss your treatment options with you. Complications from retinal vein occlusions include macular edema, neovascularization, neovascular glaucoma and detached retina. The complications can be vision-threatening. Therefore, once you have been diagnosed with BRVO or CRVO, your doctor will closely monitor your vision. In some cases, this could require monthly examinations. Your vision is one of your most valuable assets, and you should closely adhere to your scheduled examinations.